|
| Readings from Robbins Basic Pathology, 11th ed |
| Pages |
Topics |
| 57 - 76 |
Hyperemia -through- Stages of Shock |
| 276 - 292 |
Blood Pressure Regulation -through- Noninfectious Vasculitis |
| 383 - 388 |
Bleeding Disorders -through- Coag Disorders |
|
|
Website Cases:
CASE NUMBER 4
--Click here for a video debrief of the pathology findings presented in this case--
Clinical History: A 44-year-old woman with a BMI of 35 with a longstanding history of uncontrolled type II diabetes presents to the emergency department with a 1-week history of worsening left foot pain.
On exam: height 5'6", weight 225 lbs, BP 150/92, HR 97, RR 18, O2 98% on room air. Cardiovascular exam shows a regular rate and rhythm. Lungs are clear to auscultation bilaterally. Abdomen is soft, nontender. There is trace bilateral edema with loss of hair on the shins. Image of toes of left foot is shown below.
Image Gallery:
Summary of Clinical Findings
The second and third toes show gangrenous necrosis: coagulative necrosis of multiple tissue layers. This is due to ischemia secondary to advanced atherosclerosis of the medium-sized arteries of the lower extremities.
|
Clinical image questions:
- Describe the clinical findings on exam of the patient’s foot.
- Which type of necrosis is this?
4-1. Based on the findings thus far, what is the differential diagnosis?
--ANSWER--
Clinical History (continued): Laboratory tests were performed with the following results:
CBC and BMP are unremarkable.
Lab |
Value |
Reference Range |
| Hemoglobin A1c |
10% |
<5.6% |
| Fasting blood glucose |
250 mg/dL |
70-110 mg/dL |
| Total cholesterol |
304 mg/dL |
<200 mg/dL |
| LDL cholesterol |
210 mg/dL |
<100 mg/dL |
| HDL cholesterol |
28 mg/dL |
>40 mg/dL |
| Triglycerides |
300 mg/dL |
<150 mg/dL |
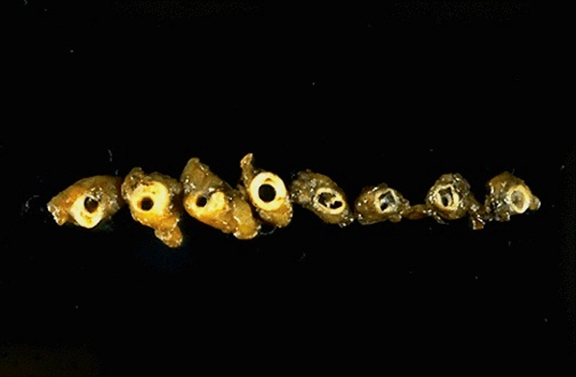
The patient was admitted to the hospital, given IV antibiotics, and a left below knee amputation is scheduled. Unfortunately, she expires during the procedure. An autopsy was performed. Sections show cross sections of left anterior descending coronary artery, proximal to distal.
Virtual slide 12 (courtesy of UMich)
[DigitalScope]
Image Gallery:
Review Vascular Histology
Muscular Arteries and Veins
UMich Slide 42 (mesentery, H&E) WebScope
UMich Slide 95M (mesentery, trichrome-elastin) WebScope
Slides 42 and 95M are mesentery spreads that contain numerous excellent examples small muscular arteries and their companion veins. Study the arteries first in slide #42 [example] , and/or #95 (trichrome) [example] . Note the thin intima, the distinct internal elastic lamina (IEL) and the media composed of circularly oriented smooth muscle cells. The media also contains some elastin and abundant “reticular” collagen, as well as specific proteoglycans. There is sometimes a condensation of elastic fibers in the outer portion of the media that may be an “external elastic lamina”, which varies from artery to artery. The adventitia is the dense, irregular connective tissue surrounding the media that varies in thickness. Remember that in blood vessels the components of the media are arranged circularly, while those of the adventitia are oriented longitudinally. In vessels where the media is too thick to be supported by simple diffusion, vasa vasorum (e.g. shown here in slide 95M) may also be observed in the adventitia.
The structure of the companion veins in slide #42 [example] and/or #95 (trichrome) [example] is less regular and may be difficult to understand at first, but still consists of the same basic layers as arteries with a tunica intima, media, and an adventitia, although the media is usually much less muscular and less organized compared to the companion artery. Conversely, the adventitia is usually thicker in veins and may often have some bundles of longitudinal smooth muscle [example] as well as vasa vasorum [example] . In some sections, you may be able to see a thin internal elastic lamina beneath the venular endothelium (particularly in slide #95M).
|
Summary of Gross Findings
Cross sections of the left anterior descending coronary artery demonstrate marked atherosclerosis with narrowing, more pronounced in the more proximal portion of this artery. In general, the worst atherosclerosis is proximal, where arterial blood flow is more turbulent. More focal lesions mean that angioplasty or bypass can be more useful procedures.
|
Summary of Microscopic Findings
Approximately 2/3 of the original lumen is filled with atherosclerotic plaque characterized by foam cells (macrophages that are filled with cholesterol. There are areas of cholesterol clefts that consist of extracellular cholesterol. The lipids are extracted during tissue processing, leaving large empty spaces. Calcification is also present as amorphous deposits of basophilic debris. This is dystrophic calcification which, as you will recall, is associated with areas of necrosis.
|
Gross questions:
- Describe the gross findings in the patient’s coronary artery.
- The proximal end is to the left and the distal end to right. Where is the lesion more prominent? Why might this be the case?
VM questions:
- Describe the histologic findings.
- On annotated screenshots, identify:
- an area of calcification, which type of calcification is this?
- intimal thickening
- foam cells
- cholesterol clefts
- the necrotic core and the fibrous cap of the lesion.
4-2. Based on these additional findings, what is the definitive diagnosis?
--ANSWER--
4-3. List 5 risk factors for the development of atherosclerosis:
--ANSWER--
4-4. Which of the following characteristics of atherosclerotic plaques is associated with the GREATEST risk of rupture?
- Abundant smooth muscle cells
- Minimal extracellular lipid
- Rare foam cells
- Scattered inflammatory cells
- Thin fibrous cap
--ANSWER--
CASE NUMBER 28
[DigitalScope]
--Click here for a video debrief of the pathology findings presented in this case--
Clinical History: A 27-year-old woman was brought to the Emergency Department following a loss of consciousness. On presentation, her BP was 111/67 mmHg in her right arm and 89/54 mmHg in her left arm. Her heart rate was 116 beats per minute. O2 sat was 93% on room air. Cardiovascular exam showed a tachycardic rate with regular rhythm. Lungs were clear to auscultation bilaterally. Neurological exam showed no focal findings. She was sent for a CT of her chest with contrast. While she was undergoing a chest CT, she became hypotensive and unresponsive and died.
Image Gallery:
Review Aorta Histology
Slide No. 9 Aorta
[WebScope]
The aorta is a large elastic artery. The luminal surface is lined by flat endothelial cells. This is called the “intima”. Adjacent to the intima is the internal elastic lamina. This is composed of elastin and has a corrugated appearance on histological section. Adjacent to the internal elastic lamina is the tunica media which is composed of smooth muscle. Finally, the outermost layer is the adventitia which is composed of connective tissue.
|
Summary of Gross Findings
At the top left of the image, there is a focus of cardiac muscle. An aortic dissection begins just distal to this point (at the aortic root) and continues through the ascending, descending and abdominal aorta as shown in the next two images. There is minimal atherosclerosis.
|
Summary of Radiologic Findings
A chest CT shows pericardial effusion (asterisk) and abdominal aortic dissection (arrowhead).
|
Summary of Microscopic Findings
There is a blood-filled tear between the inner 2/3 and outer 1/3 of the media. Note necrosis and deposition of fibrin along the margins of the defect. The remainder of the media contains the changes of "cystic medial necrosis.
|
Gross Questions
- This gross image is a tricky one to orient (explanation will be in VM video): the aorta was opened laterally and one renal artery has been bisected (midway through the close up image). With this information, please identify in a screenshot the celiac trunk and superior mesenteric artery.
Radiology Questions
- In the CT image, what is the process that is occurring in the area of the asterisk?
- What do you think is going on in the area of the black arrowhead/triangle?
- In which vessel is the black arrowhead/triangle?
VM Questions
- In the microscopic image, which is the luminal surface?
- Which is the adventitial surface?
- Identify an example of vasa vasorum.
28-1. Based on the findings thus far, what is the differential diagnosis?
--ANSWER--
28-2. Which of the following is MOST COMMONLY associated with this diagnosis?
- Antithrombin III deficiency
- Atherosclerosis
- Hypertension
- Syphilis
- Vitamin C deficiency
--ANSWER--
28-3. Which of the following should be suspected in this patient?
- Bacterial sepsis
- Connective tissue abnormalities
- Fat embolism
- Heroin use
- Hyperlipidemia
--ANSWER--
CASE NUMBER 158
[DigitalScope]
--Click here for a video debrief of the pathology findings presented in this case--
Clinical History: A 63-year-old man presented to the emergency department with a two-day history of severe chest pain and dyspnea. He had been discharged from the hospital one week earlier following a colon resection due to obstruction from a colonic adenocarcinoma that had also metastasized to the liver. Past medical history was significant for congestive heart failure secondary to hypertension. While he was in the emergency department, he collapsed and died. Gross and microscopic images from the autopsy are provided.
Image Gallery:
|
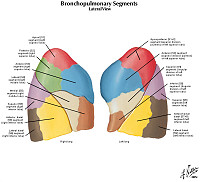
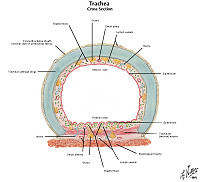
Review Lung Histology
Slide No. 24 Lung
[DigitalScope]
The primary function of the lung is gas exchange. Therefore, alveoli have thin walls lined by thin flat pneumocytes and endothelial cells. There is no thickening or fibrosis of the interstitium. The bronchioli are lined with basally oriented ciliated columnar epithelium. The bronchi are lined by similar epithelium. There are mucous glands within the submucosa. The bronchial smooth muscle is not hypertrophied. The pulmonary vessels are patent with no evidence of intimal thickening or muscular hyperplasia.
|
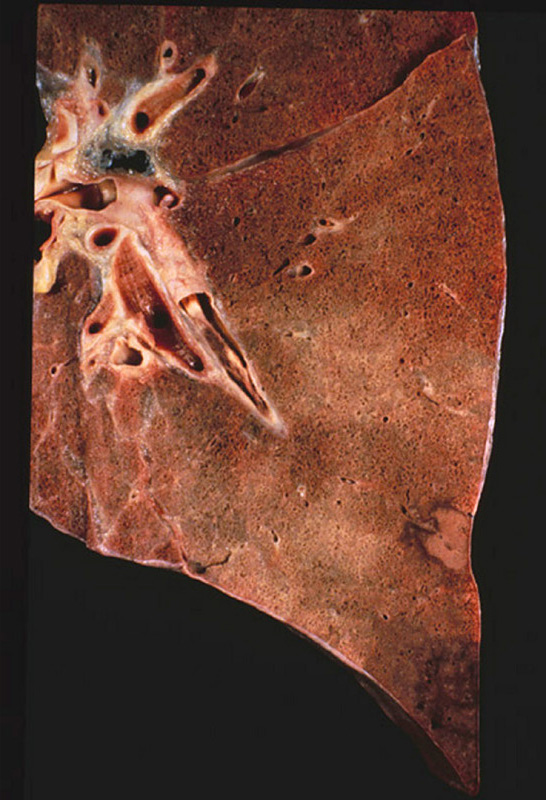
Summary of Gross and Lab Findings
The lung was dark red and heavy, and a large amount of hemorrhagic frothy fluid exuded freely from the cut surface. In the main pulmonary artery there was a large red firm clot. Many small blood clots were present in the vessels of the upper and lower lobes. Associated with these were many wedge-shaped, firmer areas in the lung parenchyma.
|
Summary of Microscopic Findings
There are two sections on the slide. On one section there are organizing thrombi in the pulmonary arteries. On the other section there is a large hemorrhagic area in which some alveolar septa are pink, smudgy, and necrotic. In other portions of the lung the septa are thickened with fibrosis.
|
Gross Questions
For the first gross image of the lung:
- Take a screen show and annotate an area of normal and abnormal lung.
- Describe the abnormal areas and what features support your findings and what the abnormal areas may represent.
- Identify a lymph node.
For the second gross image:
- identify the structures present
- any abnormal gross pathology you see present.
VM Questions
For the VM image, take a screen at scanning magnification and annotate:
- an area of normal-appearing alveolar parenchyma
- an airway
- a blood vessel
- an arterial thrombus, showing at higher magnification lines of Zahn and areas of fibroblast ingrowth
- areas demonstrating early coagulative necrosis
158-1. What is the differential diagnosis?
--ANSWER--
158-2. What do the firm, red, wedge-shaped areas of the lung MOST LIKELY represent?
- Angiosarcoma
- Hemorrhage
- Infarcts
- Metastatic disease
- Thrombosis
--ANSWER--
158-3. In cases of deep venous thrombosis with embolism, which vessels are MOST OFTEN occluded?
- Bronchial arteries
- Bronchial veins
- Inferior vena cava
- Pulmonary arteries
- Pulmonary veins
- Superior vena cava
--ANSWER--
158-4. Pulmonary emboli are more common than pulmonary infarcts. Which of the following BEST explains this observation?
- Coagulation is slower in oxygenated tissue
- Lung tissue has increased numbers of mitochondria
- Lungs have a dual arterial supply
- Oxygenation can occur across the bronchial wall
- Venous drainage is accelerated in lung tissue
--ANSWER--
CASE NUMBER 514
(no virtual slides for this case)
Clinical History: A 28-year-old woman presents to the Emergency Department with an acute onset of severe dyspnea after disembarking from a trans-Atlantic flight. She reports left-sided chest pain on inspiration. She has no significant medical history, but states that she takes oral contraceptive pills. Physical exam shows 20 breaths per minute and a heart rate of 125 bpm. Her left calf is swollen and warm. A duplex ultrasound demonstrates a deep venous thrombosis. Laboratory analysis reveals a positive activated protein C resistance test; remaining studies are noncontributory.
Image Gallery:
Clinical Image question:
- Describe the findings shown in the image and their relevance to the case vignette.
514-1. What is the differential diagnosis for her hypercoagulable state?
--ANSWER--
514-2. Which of the following is MOST ACCURATE about this disease?
- Homozygotes have a 50-fold increase in relative risk of venous thrombosis
- Inheritance is typically autosomal recessive
- It is associated with increased prothrombin levels
- Partial thromboplastin time is typically prolonged
- There is an increased incidence in patients with systemic lupus erythematosus
--ANSWER--
514-3. Which of the following is the pathophysiology of this disease?
- Autoantibodies cause platelet aggregation
- Factor V is resistant to cleavage
- Prothrombin is resistant to cleavage
- Thioester linkages form between homocysteine metabolites and proteins
- Ultra large von Willebrand multimers are found in the serum
--ANSWER--
514-4. Genetic analysis would MOST LIKELY show which of the following?
- A chromosomal translocation
- A missense mutation
- A nonsense mutation
- A partial deletion of chromosome 12
- Ring chromosomes
--ANSWER--
Review Items
THROMBOSIS, HEMOSTASIS, EDEMA, and SHOCK - Key Vocabulary Terms
HEMODYNAMICS AND ARTERIOSCLEROSIS - Key Vocabulary Terms
GOALS and LEARNING OBJECTIVES
Goal 1: Hemodynamics and Shock
Apply knowledge of the biochemical and cellular physiology to discuss the pathogenic mechanisms resulting in alterations in hemodynamics and shock. Describe the resulting pathology at the cellular, tissue and organism level and describe clinical manifestations associated with these pathologic changes.
- Objective 1: Edema
Describe the pathophysiologic categories of edema and compare and contrast, with examples, how edema can be produced as a result of changes in hydrostatic pressure or plasma oncotic pressure.
- Objective 2: Hyperemia and Hemorrhage
Explain the clinical, morphological, and physiological significance of hyperemia, congestion and hemorrhage.
- Objective 3: Shock
Classify different types of shock according to etiology and compare and contrast the pathogenesis of these different types.
Goal 2: Clotting and Disruption of Blood Flow
Apply knowledge of the biochemical and cellular physiology to discuss pathogenetic mechanisms that result in alterations in blood clotting or other disruptions to blood flow. Describe the resulting pathology at the cellular, tissue and organism level and the clinical manifestations associated with these pathologic changes.
- Objective 1: Blood Clotting
Discuss the vascular, cellular and humoral events involved in blood clotting, and provide examples of genetic or acquired factors that can lead to either excess clotting or bleeding.
- Objective 2: Thrombosis and Thromboembolism
Compare and contrast thrombosis in situ and thromboembolism with respect to sites of involvement, risk factors, and attendant pathologic and clinical consequences.
- Objective 3: Embolism
Compare and contrast the etiology and clinical consequences of different types of embolism
Goal 3: Platelets
Apply knowledge of platelet structure and function to discuss qualitative and quantitative disorders leading to abnormal bleeding.
- Objective 1: Platelets in Hemostasis
Summarize the role played by platelets in hemostasis, including platelet adhesion, activation, and aggregation.
- Objective 2: Thrombocytopenia
Identify the examples of each of the following pathogenetic categories of thrombocytopenia: decreased production, decreased platelet survival, sequestration, dilutional effect.
- Objective 3: Thrombocytopenic Syndromes
Compare and contrast the following thrombocytopenia syndromes: immune thrombocytopenic purpura, drug-induced thrombocytopenia, heparin-induced thrombocytopenia.
- Objective 4: Thrombocytopenic Purpura
Compare and contrast thrombotic thromobocytopenic purpura with hemolytic uremic syndrome.
Goal 4: Hemostasis
Apply knowledge of normal hemostasis, interaction of platelets, and procoagulant and anticoagulant factors to describe qualitative and quantitative disorders leading to abnormal bleeding and thrombosis.
- Objective 1: Types of Hemorrhage
Distinguish among the following manifestations of hemorrhage: hematoma, petechiae, purpura, and ecchymoses.
- Objective 2: Stages of Hemostasis
Compare and contrast the following stages of hemostasis: vasoconstriction, primary hemostasis, secondary hemostasis, and antithrombotic counterregulation.
- Objective 3: Secondary Hemostasis
Outline the process of secondary hemostasis, in terms of intrinsic pathway, extrinsic pathway, common pathway, fibrin formation, and fibrinolysis.
- Objective 4: Proteases and the Coagulation Cascade
Describe how particular proteins that regulate the proteases to activate the clotting cascade either promote or inhibit coagulation.
- Objective 5: Mechanisms of Hypercoagulability
Compare and contrast the roles of endothelial injury, stasis, and alterations in the regulation of blood clotting in the development of the hypercoagulable state.
- Objective 6: Risk Factors for Thrombophilia
Give examples and discuss the pathophysiology of inherited versus acquired conditions that increase the risk of thrombophilia.
- Objective 7: Disseminated Intravascular Coagulopathy
Discuss disseminated intravascular coagulopathy (DIC) in terms of etiologies, pathogenesis, clinical presentation, and course.
- Objective 8: Inherited Hemophilia
Discuss the pathogenesis and clinical and laboratory manifestations of hemophilia A and explain how it differs from hemophilia B.
- Objective 9: von Willebrand Disease
Compare and contrast types I, II, and III von Willebrand disease and explain the quantitative or qualitative abnormalities and the laboratory features observed in each type.
- Objective 10: Heparin-Induced Thrombocytopenia
Explain the mechanism of heparin-induced thrombocytopenia/thrombosis and describe its clinical presentation and approach to therapy.
Goal 5: Mechanisms of Atherosclerosis
Apply knowledge of immunologic principles, inflammation, and tissue repair to explain atherosclerosis and its complications.
- Objective 1: Factors Contributing to Endothelial Injury
Explain how environmental factors (including elevated cholesterol and LDL complexes, infection, and smoking) can contribute to endothelial cell injury.
- Objective 2: Feedback in Endothelial Damage
Describe the positive feedback loop in which damaged endothelial cells cause further endothelial damage.
- Objective 3: Atherosclerosis Plaque Rupture
Predict the local and distant consequences that are likely to follow rupture of an atherosclerotic plaque and the resultant clinical presentation.
- Objective 4: Vascular Aneurysm
Describe the morphologic changes in atherosclerosis and discuss how atrophic changes in the vessel wall may result in aneurysm formation.
Goal 6: Vascular Damage and Thrombosis
Apply knowledge of the cellular response to injury and basic hemodynamic principles to explain how defective or excessive inflammatory and reparative processes damage blood vessels and how this damage results in thrombus formation.
- Objective 1: Thrombus Formation
Discuss the steps in thrombus formation and its predisposing factors.
- Objective 2: Aortic Aneurysm and Dissection
Compare and contrast aortic aneurysms and aortic dissections in terms of their predisposing factors, the sites of involvement, and patient populations likely to be affected.
- Objective 3: Abdominal Aortic Aneurysm
Describe the clinical consequences of an abdominal aortic aneurysm.
|
|
|